Vital Signs Are Vital: How We Learned To Measure Blood Pressure.
Posted on | April 1, 2025 | No Comments
Mike Magee
It has been estimated that a medical student learns approximately 15,000 new words during the four years of training. One of those words is sphygmomanometer. the fancy term for a blood pressure monitor. The word is derived from the Greek σφυγμός sphygmos “pulse”, plus the scientific term manometer (from French manomètre).
While medical students are quick to memorize and learn to use the words and tools that are part of their trade, few fully appreciate the centuries long efforts, to advance incremental insights, discoveries, and engineering feats that go into these discoveries.
Most students are familiar with the name William Harvey. Without modern tools, he deduced from inference rather than direct observation that blood was pumped by a four chamber heart through a “double circulation system” directed first to the lungs and back via a “closed system” and then out again to the brain and bodily organs. In 1628, he published all of the above in an epic volume, De Motu Cordis.
Far fewer know much about Stephen Hales, who in 1733, at the age of 56, is credited with discovering the concept of “blood pressure.” A century later, the German physiologist, Johannes Müller, boldly proclaimed that Hales “discovery of the blood pressure was more important than the (Harvey) discovery of blood.”
Modern day cardiologists seem to agree. Back in 2014, the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure reported that “With every 20 mm Hg increase in systolic or 10 mm Hg increase in diastolic blood pressure, there is a doubling risk of mortality from both ischemic heart disease and stroke.”
But comparisons are toxic. No need to diminish Harvey who correctly estimated human blood volume (10 pints or 5 liters), the number of heart contractions, the amount of blood ejected with each beat, and the fact that blood was continuously recirculated – and did this all 400 years ago. But how to measure the function, and connect those measurements to an amazingly significant clinical condition like hypertension, is a remarkable tale that spanned two centuries and required international scientific cooperation.
Harvey was born in 1578 and died in 1657, twenty years before the birth of his fellow Englishman, Stephen Hales. Hales was a clergyman whose obsessive and intrusive fascination with probing the natural sciences drew sarcasm and criticism from the likes of classical scholar and sometimes friend, Thomas Twinning. He penned a memorable insult laced poem in Hales’ honor titled “The Boat of Hales.”
“Green Teddington’s serene retreat
For Philosophic studies meet,
Where the good Pastor Stephen Hales
Weighed moisture in a pair of scales,
To lingering death put Mares and Dogs,
And stripped the Skins from living Frogs,
Nature, he loved, her Works intent
To search or sometimes to torment.”

The torment line may be well justified in light of Hales own 1733 account of his historic first ever mention of the measurement of arterial blood pressure, illustrated and self-described here:
“In December I caused a mare to be tied down alive on her back; she was fourteen hands high, and about fourteen years of age; had a fistula of her withers, was neither very lean nor yet lusty; having laid open the left crural artery about three inches from her belly, I inserted into it a brass pipe whose bore was one sixth of an inch in diameter … I fixed a glass tube of nearly the same diameter which was nine feet in length: then untying the ligature of the artery, the blood rose in the tube 8 feet 3 inches perpendicular above the level of the left ventricle of the heart; … when it was at its full height it would rise and fall at and after each pulse 2, 3, or 4 inches.”
Having established the existence of “blood pressure,” the world would wait nearly another century to gain access to a reliable tool for measurement. That advance came from the hands of French physician-physicist, Jean Léonard Marie Poiseuille. He was born in 1799, amidst the flames of the French Revolution. In 1828, as a doctoral candidate, his dissertation on the use of a mercury manometer, attached to an anticoagulant laced cannula, in lab animal vessels as small as 2 mm in diameter, yielded measurable, and reproducible arterial pressure readings, earning him a gold medal from the Royal Academy of Medicine.
Carl Ludwig, a 31-year old German professor of physiology, next decided Poseuille needed a permanent and transportable record. His solution in 1847 was to attach a float with a writing pen to the open mercury column. As the mercury rose, the pen scratched out a reading on a revolving smoked drum.
But direct arterial puncture was impractical and invasive. By 1955, scientists had surmised that applying external counter pressure to an artery could obliterate the pulse below the obstruction, and that measuring the pressure generated by an obstructing external rubber ball would essentially reveal the blood pressure generated by a contracting heart – the systolic pressure.
In 1881, an Austrian physician named Karl Samuel Ritter von Basch created an elaborate portable machine that included a manometer capable of measuring the internal water pressure inside an inflatable rubber ball applied at the wrist to the radial artery. The pressure necessary to eliminate the pulse below was roughly the peak pressure of the column of blood when the heart contracted. Eight years later, the French physician, Pierre Carle Édouard Potain, replaced the water with air for compression.
By 1896, blood flow was appreciated as a series of waves that peaked when the heart contracted, and fell as the heart relaxed. The wrist compressing rubber rubber cup was replaced by an air filled cuff wrapped around the upper arm which constricted the larger brachial artery. A Russian surgeon, N.C. Korotkoff, in 1905, suggested that doctors listen to the waves rather than feel for the pulse. The sounds he described became known as Korotkoff sounds.
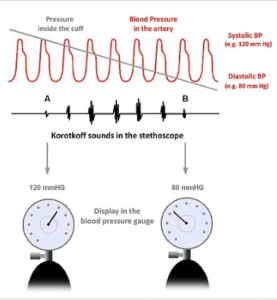
As described in a 1941 translation of the Russian paper and illustrated here by wikipedia, Korotkoff wrote, “On the basis of this observation, the speaker came to the conclusion that a perfectly constricted artery under normal conditions, does not emit any sounds…The sleeve is put on the middle third of the arm; the pressure in this sleeve rises rapidly until the circulation below this sleeve stops completely. At first there are no sounds whatsoever. As the mercury in the manometer drops to a certain height, there appears the first short or faint tones, the appearance of which indicates that part of the pulse wave of the blood stream has passed under the sleeve…Finally all sounds disappear. The time of disappearance of the sounds indicated the free passage or flow of the blood stream… Consequently, the reading of the manometer at this time corresponds to the minimum (diastolic) blood pressure.”
It is easy to forget, in an age of semiconductors, photocells and strain gauges, that progress in understanding the human circulatory system took centuries to acquire, and international cooperation. When Covid hit, homes that could acquired Home Blood Pressure Monitors and Pulse Oximeters that attached to an index finger and delivered oxygen saturation of blood and pulse with no delay. For a little more, you can access a Portable ECG monitor in the comfort of your own home.
We appear to have entered a new era, one where a U.S. president and his enablers are fast at work dismantling American scientific capacity and cooperative, AI-laced, international science discovery capacity. The timing couldn’t be worse, since increasingly, we patients are expected to enthusiastically participate as both providers and recipients of our own health care.
Tags: blood pressure > blood pressure monitor > ECG monitor > Jean Leonard Marie Poiseuille > Karl Samuel Ritter von Basch > Korotkoff sounds > N.C. Korotkoff > Pierre Carle Edouard Potain > pulse oximeter > sphygmomanometer > Stephen Hales > william harvey
Comments
Leave a Reply


